No child should die of choking. Yet every day children choke, and every year hundreds die and thousands land in emergency departments. One of every parent’s biggest fears is seeing their child choking. Knowing what to do in this situation could be the difference between life and death for loved ones.

Choking among school-aged children is on the rise. Choking on food and small objects is a leading cause of death in children under the age of 5. Young children may not have fully developed muscles for chewing, enough teeth, or the ability to chew and swallow certain foods thoroughly. Toddlers explore their world by putting things in their mouths and their airways are very small in diameter. These traits and behaviors make them vulnerable to choking on foods and small objects that can lodge in the throat and block the airway.
Choking is largely preventable with a little knowledge and by following proven guidelines. But knowing what to do if a child’s airway becomes blocked is equally important.
82% of parents would not know what to do if there child choke, burned themselves or even stopped breathing.
While you can’t predict when an emergency will occur, you can be prepared. In less time than you think, First Aid to Save a Life can give you the vital knowledge and skills you’ll need to respond to a life-threatening situations like choking with confidence.
How to recognize?
In a choking emergency, quick recognition and action are keys to clearing a blocked airway successfully. when the airway becomes blocked, a child will instinctively begin coughing to clear the blockage and may grasp at the throat.
Other signs of choking may include:
Coughing may be forceful, or weak with wheezing noises.
The child’s skin color may change.
The child may have a look of panic on his/her face.
The child may not be able to cough at all, speak, cry, or breathe.
If the child is not able to cough, speak, cry, or breathe, you must act fast to clear the airway. These signs are an indication of severe choking. All other signs listed above are indicating mild choking.
Alert:
Make sure it is safe for you to help. Get consent if parent/guardians are present and unable to help. Ask for help if no one is present and choking patient is conscious, for rest of the cases implied consent authority will prevail.
Types of Choking:
Mild Airway Obstruction: If a choking child is coughing forcefully, you should encourage coughing, observe closely, and not interfere. But be ready to help if the child/s condition gets worse, such as if the child is not able to clear the blockage with coughing, or can’t breathe.
Severe Airway Obstruction: if the child can’t cough, speak, cry, or breathe, you should have someone else call EMS, while you give first aid for choking.
Don’t wait for help to arrive or delay care. A child in this condition is not getting any oxygen and needs immediate care. If you are lone rescuer, you should give first aid for choking to clear the airway, and then call EMS.
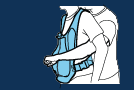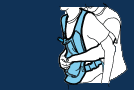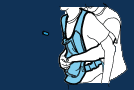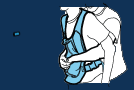
Child Anti-Choking Technique (Abdominal Thrusts/Heimlich Maneuver):
1:- Ask for help (illustrated above).
2:- Wrap your arms around the child’s waist, and find the child’s belly button with one or two fingers.
3:- Next, make a fist with the other hand and place it flat, thumbside against the child’s stomach, just above your fingers(s) and below the lower tip of the child’s breastbone.
4:- Cover your first with the other hand.
5:- Give quick, inward and upward thrusts until the airway is clear.
6:- Monitor the child until help arrives, and ensure follow-up medical care to assess for possible injury.
If the child becomes unresponsive………….
Help the child to the ground, face-up.
If alone, provide 2 minutes of CPR before activating EMS yourself.
Begin CPR starting with compressions (chest compression + ventilation) if you are trained. If not, seek guidance from EMS and do compression-only CPR. Look in mouth for an object before giving rescue breaths. Remove any object seen. Continue CPR until child shows obvious signs of life, or another provider or EMS personnel take over.
Infant Anti-Choking Technique (Chest Thrusts/Back Blows):
1:- Assess Infant:
Look at infant’s face. If infant has weak, ineffective coughs, or lack of sound even when clearly attempting to breathe, act quickly! If available, have a bystander activate EMS.
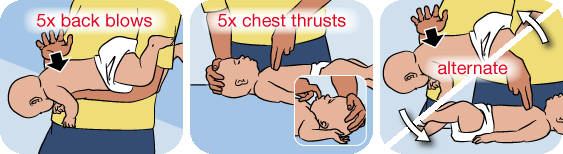
2:- Give 5 Back Blows:
Lay infant face down over your forearm with legs straddled and with head lower than the chest. Support the head by holding the jaw. Using heel of other hand, give 5 back blows between the shoulder blades.
3:- Give 5 Chest Thrusts:
Sandwich infant between your forearms and turn onto back. Place 2 fingers on breastbone just below the nipple line and give 5 chest thrusts. Repeat back blows and chest thrusts until infant can breathe normally.
If infant becomes unresponsive…………
Gently place infant on firm surface. If alone, provide 2 minutes of CPR before activating EMS yourself.
Begin CPR starting with compressions. Look in mouth for an object before giving rescue breaths. Remove any object seen. Continue CPR until infant shows obvious signs of life, or another provider or EMS personnel take over.
FATSAL is a training, consultancy and sales company working since 2011 with a mission to train people to prevent injuries/illness and save lives. We strive to make first aid part of everybody’s life. We use best training supplies during our sessions to make learning easy and enhance its retention. For choking we use Act+Fast Medical’s Anti-Choking Trainer (an educational medical device patent in US) to educate participants, parents, teachers, as well as the children themselves, to learn these simple life-saving techniques. Practicing with this product will provide the confidence to react during an emergency and save lives. Use this trainer to teach yourself and everyone you know, and help make the world a little safer.
For Your Safety,
Faisal Javed Mir & First Aid to Save a Life
Did you like the post? Let’s get connected on Facebook, LinkedIn, Twitter & YouTube.
You might also like:
MEDIC First Aid International – Instructor Development Course
First Aid for Small Businesses
Family First Aid
Upcoming Training Courses